 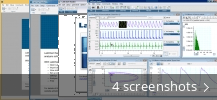
We also investigated the area under the curve that defines the total relaxation over the experiment. The maximum relaxation (Rmax Figure 4B) was not reduced by esomeprazole compared with the control noting the controls and treated arteries reached maximum relaxation at different concentrations.  
Further, the maximum relaxation achieved by esomeprazole treatment compared with the control was determined. Both esomeprazole MTH ( p = 0.0012) and esomeprazole MH ( p < 0.0001) treatment induced significant relaxation of pre-constricted arteries compared with control (vehicle) ( Figure 4A), when administered at the highest concentration (100 μmol/L). Wire myograph ex vivo experiments were performed. Maternal omental arteries were isolated from omental fat tissue obtained at caesarean section from healthy individuals at term. We next examined whether esomeprazole MTH had vasoactive properties. Systemic vasoconstriction and hypertension are hallmark features of preeclampsia. Collectively, our pre-clinical studies suggest that the PPIs, particularly esomeprazole, could be effective in treating preeclampsia. Subsequently we explored the efficacy of combining esomeprazole with other potential candidate therapies and demonstrated that combining esomeprazole treatment with the candidate preeclampsia therapeutics, metformin or sulfasalazine, additively reduced sFLT-1 secretion and markers of endothelial dysfunction. Using ex vivo studies, we demonstrated that esomeprazole directly induced vasodilation of omental arteries and reduced blood pressure in a mouse model of preeclampsia. Esomeprazole treatment reduced cytokine release from placenta and endothelial cells. Esomeprazole, rabeprazole, and lansoprazole reduced markers of endothelial dysfunction and upregulated antioxidant cytoprotective molecules. In in vitro studies, the PPIs esomeprazole, lansoprazole, rabeprazole, omeprazole, and pantoprazole significantly reduced secretion of anti-angiogenic factors, including sFLT-1 (which is markedly upregulated in preeclampsia) from primary human placental tissue and cells, including endothelium, from both normal and preeclamptic pregnancies. However, esomeprazole MH was more efficacious than esomeprazole MTH in our in vitro studies.įundamental work carried out by our team previously demonstrated that PPIs can mediate multiple aspects of the pathophysiology of preeclampsia. 
Using primary human tissues and cells, we validated that esomeprazole is effective in enhancing vascular relaxation, and can reduce key factors associated with preeclampsia, including sFLT-1 and endothelial dysfunction. Esomeprazole is safe to use in pregnancy and a candidate treatment for preeclampsia. Finally, using wire myography, we demonstrated that both compounds were able to induce vasodilation of human omental arteries at 100 µM. Neither esomeprazole MH nor MTH quenched cytotrophoblast reactive oxygen species production in response to sodium azide (ROS assay). Both drugs could mitigate expression of the endothelial dysfunction markers, vascular cell adhesion molecule-1 and endothelin-1 (via qPCR). Here, we found that both treatments reduced secretion of sFLT-1 (anti-angiogenic factor) from primary cytotrophoblast, but only esomeprazole MH reduced sFLT-1 secretion from primary human umbilical vein endothelial cells (assessed via ELISA). In this study we investigate the difference in the preclinical effectiveness between 100 µM of esomeprazole MH and its hydration isomer, esomeprazole magnesium trihydrate (MTH). Previously, we demonstrated that the proton pump inhibitor, esomeprazole magnesium hydrate (MH), could have potential as a repurposed treatment against preeclampsia, a serious obstetric condition. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
